
A platelet-rich plasma (PRP) injection is a minimally invasive therapy using a concentration of plasma, harvested from a patient’s own blood, to treat many types of sports injuries or to relieve muscle, joint, or tendon, and ligament pain, while significantly speeding up recovery. Platelet-rich plasma is known to have an increased level of growth factors, or proteins, which has proven vital for healing damaged tissue, and aids in regeneration and repair. Increased levels of these important growth factors, delivered through a PRP injection, can accelerate the body’s natural healing process by regenerating cells to repair damaged tissue. If you live in or near Tampa and would like to know if PRP Injections are an appropriate treatment for you, please contact us at 813-684-BONE.
Types of Injuries Commonly Treated with a PRP Injection
PRP injections are particularly effective for most sports injuries, chronic muscle pain, or strained tendons and ligaments, allowing individuals to return to regular activities more quickly and with less pain. These types of injuries include:
-
- Tennis or golfers elbow
- Rotator cuff injuries
- Achilles tendonitis and plantar fasciitis
- Ankle sprains
- Hip strains
- Patellar tendonitis, or jumpers knee
- Pulled hamstring muscles
- Knee sprains or strains
- Joint osteoarthritis
Contact the Tampa office of the Orthopaedic Medical Group of Tampa Bay to discuss your specific injury, and to schedule an evaluation appointment to determine if a PRP Injection will help you heal more quickly.
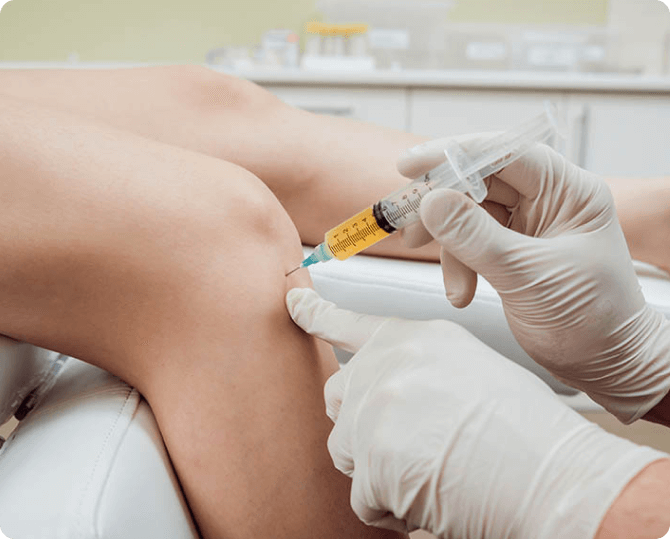
PRP Injection Procedure
- Similar to a routine blood test, a small amount of blood is drawn from the patient.
- The blood sample is placed into a centrifuge to separate platelet-rich plasma from red blood cells.
- The platelet-rich plasma is transferred to a syringe.
- Using ultrasound guidance to pinpoint the precise location, the doctor will inject the platelet-rich plasma into the injured area.
The PRP injection is an in-office procedure, and usually takes under an hour.
- Patients may notice an increase in swelling, bruising or pain of the injured area immediately following the injection. Usually, these symptoms improve as the injury heals.
- Patients are usually advised to limit or avoid any activity that may put a strain on the injury.
- For up to four weeks post treatment, patients must avoid the use of non-steroidal anti-inflammatory (NSAIDS) drugs. Your doctor may recommend other types of pain medication.
- As with any medical procedure, there may be risks, such as infection or tissue damage. Your doctor will advise you of any risks or potential side effects.
Platelet-rich plasma injection therapy provides patients with a safe and effective treatment option by using the body’s natural healing process for pain relief, long-lasting healing and the ability to return to a normal lifestyle much more quickly. If you are suffering from a sports injury, chronic muscle or joint pain, or tendon or ligament damage, please visit the contact page or call the Tampa office of the Orthopaedic Medical Group of Tampa Bay to schedule an appointment for an evaluation, and to determine if PRP Injection therapy will aid in your recovery.




