Hip & Knee
At Orthopaedic Medical Group of Tampa Bay, your care is personal, coordinated, and led by experienced shoulder specialists. From consultation through recovery, we are committed to high-quality care, clear communication, and an exceptional patient experience.
Meet Our Hip & Knee Replacement Specialists
Meet our hip & knee specialists, offering expert care with personalized attention and a truly elevated patient experience.

Jiffy Knee® Certified
Primary Hip & Knee
Replacement Specialist

Primary and Revision Hip & Knee Replacement Specialist

Primary and Revision Hip & Knee Replacement Specialist

Primary Hip & Knee Replacement Specialist
Locations

Fishhawk
13837 Circa Crossing Dr, Suite 120
Lithia, FL 33547
813-684-BONE (2663)

Plant City
420 North Plant Ave
Plant City, FL 33563
813-684-BONE (2663)

Tampa
4541 S Dale Mabry Hwy
Tampa, FL 33611
813-684-BONE (2663)

Brandon Healthplex
10740 Palm River Rd, Ste 310
Tampa, FL 33619
813-684-BONE (2663)

Apollo Beach
7239 Paradiso Drive, Suite 102
Apollo Beach, Fl 33572
813-684-BONE (2663)

St. Petersburg
2805 54th Ave N St.
Petersburg, FL 33714
813-684-BONE (2663)

Sun City
1901 Haverford Avenue, Suite 107
Sun City Center, FL 33573
813-684-BONE (2663)

Wesley Chapel
2553 Windguard Circle
Wesley Chapel, FL 33544
813-684-BONE (2663)

Winter Haven
400 Ave K SE Suite #4
Winter Haven, Fl 33880
813-684-BONE (2663)
Patient Stories & Expert Insights
Reviews
What is Total Joint Replacement Surgery?
Total Hip Replacement
A total hip replacement is a surgical procedure in which a damaged or arthritic hip joint is replaced with artificial components designed to restore smooth movement and reduce pain. During the operation, the surgeon removes the worn-out cartilage and bone from the hip joint and replaces the ball of the femur and the socket of the pelvis with prosthetic implants. These implants are typically made of metal, ceramic, and durable medical-grade plastic.
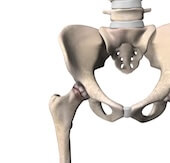
Anterior Hip Replacement
At Orthopaedic Medical Group of Tampa Bay, we offer multiple surgical approaches for total hip replacement, including the anterior approach, depending on each patient’s individual needs and anatomy. The anterior approach is a technique where the hip joint is accessed from the front of the hip rather than the side or back. In some cases, this approach may allow surgeons to work between muscles instead of detaching them, which can support early mobility and recovery.
Our surgeons take an individualized approach to hip replacement surgery and will discuss the best surgical plan based on your condition, lifestyle, goals, and overall health.
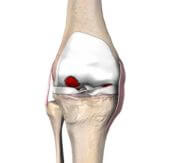
Total Knee Replacement
A total knee replacement is a surgical procedure in which a damaged or arthritic knee joint is replaced with artificial components to relieve pain and restore function. During the procedure, the surgeon removes the worn cartilage and a small amount of bone from the femur, tibia, and sometimes the patella. These surfaces are then replaced with metal and medical-grade plastic implants that recreate the smooth gliding motion of a healthy knee joint. The goal of the surgery is to reduce pain, improve stability and mobility, and allow patients to return to everyday activities.
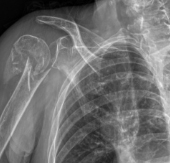
Shoulder Replacement After Fracture
In the case of a complex fracture which has caused significant joint damage, shoulder replacement may be recommended to restore stability, reduce pain, and improve shoulder function.
The Jiffy Knee® Approach
Schedule A Jiffy Knee® Consultation Today!
Scheduling Your Surgery
The Scheduling Process
At Orthopaedic Medical Group, our dedicated team is here to guide you through every step of the joint replacement process. From your initial consultation to helping you track down necessary pre-surgery test results and coordinating your postoperative follow-up, we’re committed to making the process as smooth and stress-free as possible.
Have questions? Email our team at JointReplacement@OMGTB.com, and we’ll be happy to assist you.

Preferred Surgical Facility
At Orthopaedic Medical Group Surgery Center, every aspect of your experience is thoughtfully designed around your comfort and peace of mind. Patients receive a concierge-style experience in a modern, surgeon-led facility designed for comfort, efficiency, and personalized care. From streamlined scheduling to attentive day-of-surgery support, every detail is focused on creating a smooth, high-quality experience.
Pre-Operative Testing
Once surgery is recommended, you’ll receive a packet with all required preoperative testing instructions and educational materials. Your surgical coordinator will contact you within 24–48 hours to schedule your surgery and guide you through any required testing. Most patients will need to undergo blood work, EKG, and clearances from your primary care or specialist office.
You’ll meet with your surgeon about two weeks before surgery to review results, and return to the office 2–4 weeks afterward for a postoperative visit and X-rays
Total Joint Replacement Class
Our Total Joint Replacement Class is designed to prepare you for every step of your surgery and recovery. You’ll learn what to expect before, during, and after your procedure, including tips for pain management, mobility, and safety at home. Attending this class helps reduce anxiety, improves recovery outcomes, and ensures you feel confident throughout your joint replacement journey. It’s an essential part of getting back to the activities you love safely and successfully. Classes can be taken in person and online. They are offered in Spanish and English.

Surgical Fees
Although your insurance might cover the majority of surgical costs, each plan varies based on your individual benefits. During the surgical planning process, you may encounter three types of fees: the physician fee, facility fee, and anesthesia fee. These will be explained to you over the phone prior to your surgical date, and payment will be required within 72 hours of the procedure.
PHYSICIAN FEE
This fee is collected by our office 2-3 weeks in advance:
813-684-2663 ext. 155
FACILITY FEE
This fee is collected independently by your surgical facility:
OMGSC:
813-535-6647 option 3
BayCare:
813-852-3116 option 2
ANETHESIA FEE
This fee is billed after your anesthesia is completed
OMG Anesthesia Team:
727-203-5114
BayCare:
813-852-3116 option 2
OTHER ITEMS NOT COVERED BY TRADITIONAL INSURANCE
Items like ice machines or TENS units are not covered by insurance but are essential to your recovery. These items are available for purchase in office and will be discussed during your pre-operative appointments.

Cold Therapy

TENS Unit
After Surgery
Pain Management
You should expect moderate-severe pain, swelling, bruising, and difficulties walking & sleeping for the first few weeks after surgery.
Medication prescribed BEFORE Surgery:
Journavx is a non-narcotic medication that helps reduce pain and need for opioids. It will not remove all pain but makes it more manageable. This will be sent to a pharmacy before your procedure. It may not be fully covered by insurance, although the manufacturer does offer a coupon online. The pharmacy will call to review costs and schedule delivery or pick up prior to surgery. You will take 2 pills on the morning of surgery, then 1 pill every 12 hours until the prescription is finished.
Medication prescribed on the day of surgery:
Please consult your primary care physician prior to taking any prescribed medications:
Narcotic Medication (only to be used when experiencing severe pain)
- Anti-Inflammatory: Celebrex 200mg
- Pain Medication: Tylenol 1000mg
- Stomach Protectant: Omeprazole 20mg
- Nausea Relief: Ondansetron 4mg (if needed)
- Blood Clot Prevention: Aspirin/Eliquis
Special Note:
Medication alone will NOT resolve all of your pain. The best way to manage pain is to:
- Use an ice machine & TENs unit
- Perform home exercises 2-3x a day
- Elevate your leg
Wound Care
In most cases your incision will be closed with dissolvable sutures and a white or clear mesh tape as shown. The dissolvable sutures do not require removal in office.
- 48-72 hours after surgery remove the outer dressing.
- DO NOT remove the white or clear mesh tape.
- You may now shower normally. DO NOT soak the incision under water.
- DO NOT apply lotions, creams, alcohols, peroxide, or any wound cleaning agent to the incision.
- You do not need to cover the incision once outer dressings are removed.
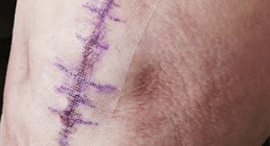
Prineo Dressing

Sylke Dressing
Bracing
Your arm will be placed in a kahuna shoulder brace after your surgery. The brace will be worn for a total of 4-6 weeks after surgery.
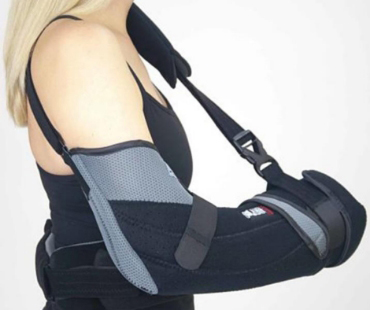
DO:
- Remove your brace to shower/for hygiene purposes.
- Remove your brace when changing clothes.
- Remove your brace to perform postoperative home exercises.
- Sleep in your brace.
DON’T:
- Don’t drive while in your brace for the first 2 weeks after surgery.
- Adjust/change strap lengths after surgery.
Physical Therapy
Physical Therapy after surgery is critical to your success. Your willingness to complete your exercises daily will have the greatest impact on your recovery. There are two types of physical therapy you may receive throughout your recovery:
HOME PHYSICAL THERAPY
NOTE: Home therapy is often used after knee replacement but isn’t essential, and it’s typically not needed for hip replacements
- Coordinated by our office!
- Your home therapy company will contact you prior to their arrival.
- Their first visit to you will be 1-3 days after surgery.
OUTPATIENT PHYSICAL THERAPY
- Coordinated by YOU!
- To start 2 weeks after surgery
- Referrals to physical therapy (PT) will be provided during your preoperative appointment.
- It is highly encouraged for you to attend one of our PT locations.
If you have Oscar, Ambetter, or Medicaid, you will not receive home therapy as it is not covered by your insurance plan. Home therapy is not essential for hip replacement patients. We encourage you to begin outpatient physical therapy no later than 1 week after surgery.
HEALTHPLEX
10740 PALM RIVER RD STE 310 TAMPA, FL
813-359-1891
ST. PETE
2805 54TH AVE N ST. PETERSBURG, FL
727-306-0459
FISHHAWK
13837 CIRCA CROSSING DR LITHIA, FL
813-536-7622
PLANT CITY
420 N PLANT AVE PLANT CITY, FL
813-730-8072
APOLLO BEACH
7239 PARADISO DRIVE, STE 101, APOLLO BEACH, FL
813-798-1367
Return to Activities
You will be up, walking, performing specific exercises, and climbing stairs the same day of your procedure, however, it can take roughly 6-12 months for your strength, and range of motion to return. Additionally, it can be normal to have pain, stiffness, or soreness for the first year after surgery. These symptoms will improve over time throughout your recovery.
Return to Driving:
Once you have stopped narcotic pain medication, and feel comfortable operating a vehicle.
Return to Swimming:
Once your incision has fully healed (roughly 6-8 weeks after surgery).
Return to Work & Sports:
Patients with seated jobs may return to work as soon as possible. Patients with active jobs, or who enjoy sports may return gradually around 2-3 months.
Full Recovery:
Can take 6-12 months. Intermittent swelling, pain, or stiffness is normal during this period.




