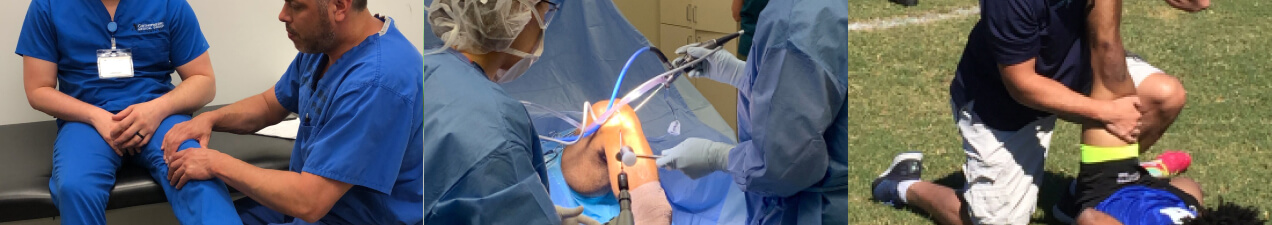
Knee Conditions, Injuries & Treatments
The ACL & PCL
The anterior cruciate ligament (ACL) is one of the primary stabilizers of the knee joint. Injuries to the ACL are very common in sports injuries, motor-vehicle accidents and falls. This injury can be treated with both non-surgical (rehab and bracing) and surgical repair or reconstruction. Each knee specialist at OMG has the education, training and expertise to provide quality care for these injuries. Most people that are active (play sports, golf, tennis, hike, bike) and work on their feet all day will typically require a surgical procedure by one an OMG knee surgeon to restore stability to the knee joint.
The PCL (posterior cruciate ligament) is another stabilizer of the knee joint along with the ACL. The PCL is not injured as often as the ACL but can be torn with severe twisting injuries in sports, hyperextension injuries, and direct blows to a bent knee. A good example can be when the knee hits the dashboard in a car accident.
Multi-Ligament Injuries
Multiple ligament knee injuries happen when more than one of the knee’s ligaments is torn. They are less common than single ligament injuries (like an ACL tear).
A ligament is a short band of tough, flexible, fibrous connective tissue that connects one bone to another bone and provides stability to a joint, like the knee. There are four main ligaments that provide stability to the knee:
- The anterior cruciate ligament (ACL)
- The posterior cruciate ligament (PCL)
- The medial collateral ligament (MCL)
- The lateral collateral ligament (LCL)
Injuries to more than one of these ligaments is called a Multi-Ligament injury and can be very serious. These types of injuries should be seen by an orthopaedic surgeon who is a knee specialist and has experience in treating these injuries.
Meniscus Tears
Each of your knees has two C-shaped pieces of cartilage that act like a cushion between your shinbone (Tibia) and your thighbone (Femur), this cartilage are called the (menisci.).
A torn meniscus is one of the most common knee injuries. Any activity that causes you to forcefully twist or rotate your knee, especially when putting your full weight on it, can lead to a torn meniscus. While these often occur in the younger more athletic population; they are very common in people over the age of 40. Thankfully small chronic tears are often non-painful and depending on your activity level; you may be able to treat small tears without surgery. Bracing and physical therapy are common methods of treating meniscus tears.
Sprains & Strains
A sprain is the medical term used to describe an injury to a ligament. Ligaments are tough bands of fibrous tissue that connect one bone to another bone; which provides stability to a joint. In the knee, ligaments connect the femur (thigh bone) to the tibia (shin bone) on the inside of the knee. The ligaments on the outside of the knee are the medial collateral (MCL) and lateral collateral (LCL).
A knee strain is the medical term used to describe an injury to a muscle or tendon around the knee joint. The most common strains, often called muscle pulls, are to the Quad (muscle in front of the leg) and Hamstring (Hammy) the muscle on the back of the leg. These injuries often happen from overuse or a sudden, dramatic increase of use of the hip and knee joints. Like running, sprinting, hiking and strenuous/heavy lifting.
Patella Dislocation
A dislocated kneecap occurs when the patella (kneecap) that sits over the front of the knee comes out of its groove at the end of the thigh bone (femur), coming to rest on the outside of the knee joint. This can cause stretching or tearing to the supporting ligaments and tendons. This is most common in young female athletes but can be caused by any twisting injury to the knee.
Knee Osteoarthritis
Osteoarthritis, commonly known as wear-and-tear arthritis, is a condition in which the natural cushioning between joints — cartilage — wears away. While age is a major risk factor for osteoarthritis of the knee, young people can get it, too. For some individuals, it may be hereditary. For others, osteoarthritis of the knee can result from injury or infection or even from being overweight.
Knee Contusions
A contusion is the medical term for bruise. It’s the result of a damaged blood vessel or capillary leaking blood into the area surrounding an injury. If you have an injury to your knee that damages the muscle or skin tissue, it’s usually referred to as a soft tissue contusion. A bone contusion, or bone bruise, to your knee is more severe, but it features many of the same symptoms as a soft tissue contusion.
Knee Fractures
The knee is the meeting place for four leg bones: the kneecap (patella), the thighbone (femur), the shinbone (tibia) and the calf bone (fibula). Damage to any of these bones can result in a fracture. Doctors categorise fractures in several different ways.
In a non-displaced fracture, the broken pieces remain in contact with each other, or just a fraction apart, leaving most of the bone intact and in its correct position.
In a displaced fracture, the pieces break and are no longer properly aligned. A comminuted fracture is where the bone breaks into many pieces. Open or closed fractures denote whether the bone has broken through the surface of the skin (open) or not (closed). The providers at OMG have extensive training in the treatment of fractures as many have training at the University of Maryland Medical Center and R Adams Cowley Shock Trauma Center.
Knee Replacement
A knee replacement (also called knee arthroplasty) might be more accurately termed a knee “resurfacing” because only the surface of the bones are replaced.
There are four basic steps to a knee replacement procedure:
- Prepare the bone: The damaged cartilage surfaces at the ends of the femur and tibia are removed along with a small amount of underlying bone.
- Position the metal implants: The removed cartilage and bone is replaced with metal components that recreate the surface of the joint. These metal parts may be cemented or “press-fit” into the bone.
- Resurface the patella: The undersurface of the patella (kneecap) is cut and resurfaced with a plastic button. Some surgeons do not resurface the patella, depending upon the case.
- Insert a spacer: A medical-grade plastic spacer is inserted between the metal components to create a smooth gliding surface.
Biologics
As healthcare continues to advance technology an increasing number of facilities and physicians have begun to offer intra-articular injections of platelet rich plasma (PRP), lipoaspirate and bone marrow aspirate concentrate as a therapeutic intervention. Studies show that these biologic therapies have been effective in treating muscle and tendon injuries, and shown benefits in patients with knee arthritis. These injections are often marketed directly to the public based on the promise of pain relief and healing of damaged cartilage. Improvements in joint function, reduction in pain, and an increase in cartilage in the affected joint are often touted as potential benefits.
These treatments can indeed improve pain and function, but should not be considered a “miracle cure” that will for certain avoid surgery or therapy. The knee specialists at OMG understand the role of these therapies, stay current on the latest research, and can identify which patients and conditions biologics are likely to be successful in treating.
Find Your Knee Surgeon
Knee Surgeon
Total Hip & Knee Replacement Specialist and General Orthopaedic Surgery
CEO & Joint Replacement Specialist and General Orthopaedic Surgery
General Orthopaedic Surgery & Sports Medicine Specialist
Sports Medicine and General Orthopaedic Surgery
Total Hip & Knee Replacement Specialist and General Orthopaedic Surgery
Subspecialty Certified Sports Medicine Specialist and General Orthopaedic Surgeon
We Accept Over 200 Insurance Plans
Related News & Articles
Not all knee replacements are in response to degenerative conditions in seniors like osteoarthritis. Sometimes, active adults under 50 years of age sustain injuries from a direct impact or show…
In this article, we delve into the intricacies of robotic knee replacement in complex cases, exploring how this innovative approach is transforming patient outcomes and quality of life.
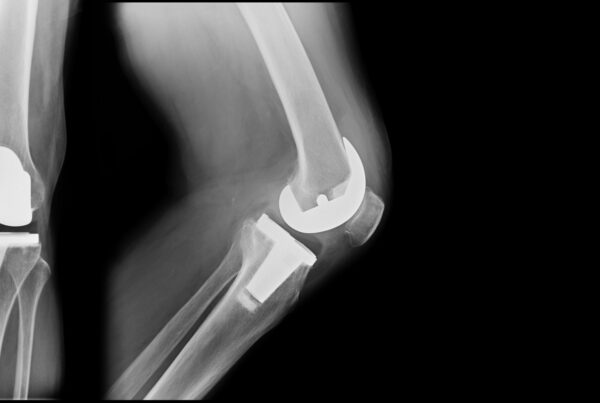
Post-knee replacement exercises are a vital component of your recovery journey, playing a crucial role in strengthening the knee, improving range of motion, and regaining mobility.

















