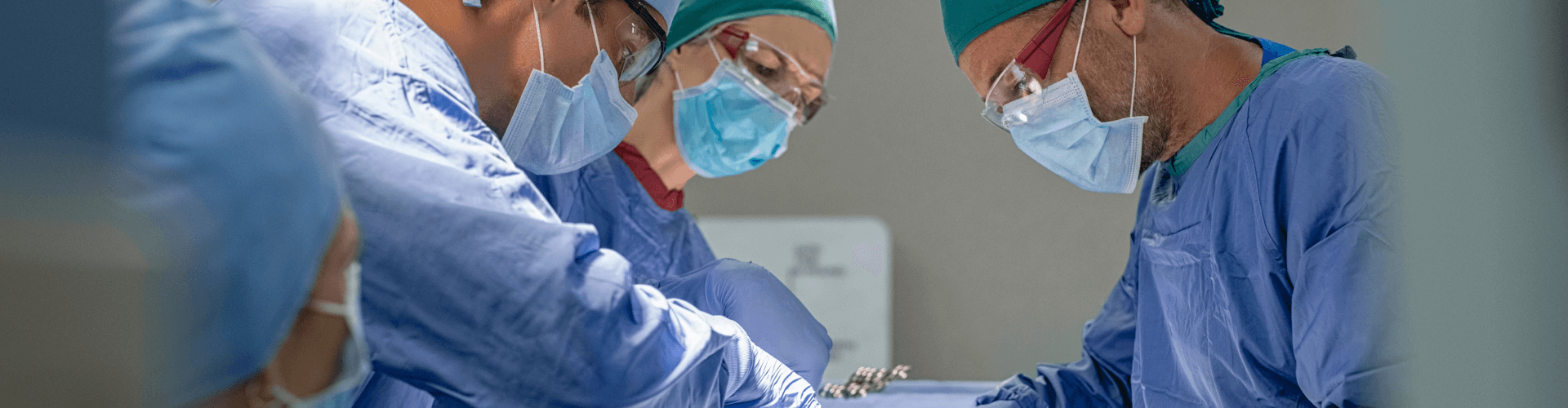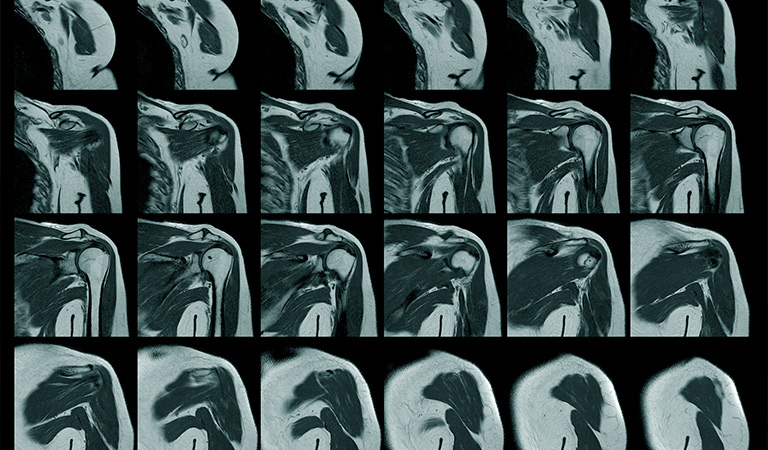
What is rotator cuff surgery?
Rotator Cuff Surgery is a procedure where the tendon or tendons of the rotator cuff are reattached to the bone of the proximal humerus, called the tuberosity.
Currently, this is done most often with an Arthroscopy, which means through multiple small incisions about 1cm in size, using a camera called an arthroscope, and instruments that go through the small incisions. Sometimes, very large tears require a bigger incision, which is called an open repair, but this is more rare as arthroscopic techniques have improved.
In order to repair the tendon back to the bone, a suture anchor is used, which essentially is an eye-let that is placed into the bone with sutures coming out of it, and the sutures are passed through the tendon and either tied or pulled- on to bring the tendon back down to the bone. There are various methods, anchors, and techniques utilized, but the primary part of the procedure is to pull the tendon back down to the bone to allow the tendon to heal. The sutures do not resorb or go away, but they get incorporated into the repair and do not cause any adverse reactions or problems.
As part of a rotator cuff procedure, there are other procedures done secondarily to help relieve pain, and these could be debridements (cleaning out of frayed or inflamed tissue), a decompression (removing bone spurs), biceps tenotomy or tenodesis (cutting the biceps or cutting and reattaching the biceps) if the biceps is torn or frayed, and a distal clavicle excision (opening up the space between the clavicle and the acromion, or the AC joint, if this is painful and arthritic). The goal always is to repair the torn rotator cuff tendon and remove anything that could be causing pain. The rate limiting factor on recovery time, however, is dictated by the rotator cuff repair itself, not these secondary procedures.
When would you need rotator cuff surgery?
Patients present usually one of two ways with rotator cuff injuries: either from a traumatic event like a fall or a traction to the arm, or pain that has slowly progressed over time from overuse. The first presentation is called a “traumatic” rotator cuff injury, and the second presentation is called an “atraumatic” rotator cuff injury.
In the past, all rotator cuff injuries and tears usually received a course of conservative measures/treatments before surgery would be offered: this would be activity modification, rest, Physical Therapy, Anti-inflammatories, and possible Cortisone injections.
If the patient did not improve within 6-12 weeks after starting treatment, then an MRI would be ordered and if there was a tear, surgery would be offered. Recently, however, we have scientific studies and evidence that patients with a “traumatic” tear have better outcomes with early surgery. For that reason patients who now present with a traumatic injury and end up obtaining an MRI which ultimately shows a rotator cuff tear, are typically offered surgery first before any conservative/non-operative treatment is administered. So, patients who end up getting surgery most likely either have a traumatic rotator cuff tear or they have tried conservative/non-operative treatment for a period of 6-12 weeks without improvement.
What does a rotator cuff tear feel like?
While the tear from the rotator cuff is in the shoulder itself, the majority of patients who have pain will feel it down the side of their arm. This is due to referred pain from the nerves that innervate the rotator cuff tendon, and these nerves also have a sensory distribution down the side of the arm; as well as the fact that the space between the deltoid and acromion (part of the scapula) versus the rotator cuff tendons, ie the Bursal Space, goes down to the mid-arm. So, when a rotator cuff tear is present, the bursa will be inflamed, and patients will feel the pain down the arm. Another symptom of rotator cuff tears is pain that is worse at night, and patients have difficulty laying on that shoulder.
The difference between tears of the tendon and other rotator cuff disorders that could mimic tears ( like bursitis, impingement, capsulitis), is that rotator cuff tears usually have a sense of weakness in the arm, especially when trying to reach out from the body or overhead with any resistance.
What are common ways rotator cuff tears happen?
Rotator cuff tears come in two forms: traumatic and atraumatic (or non-traumatic). The majority of rotator cuff tears that end up being seen by our orthopaedic surgeons are atraumatic/nontraumatic, ie without a cause.
There are risk factors for getting the atraumatic/nontraumatic tears. Risk factors that cannot be changed or modified are age (tear presence and risk increases as you get older, usually starting after the age of 55 years old), and genetics or mechanics (how the tendon is built or the biology, blood supply, and health of the tendon). Modifiable risk factors, ie factors that can contribute to the presence of a tear that can be changed or altered) are smoking, uncontrolled diabetes, repetitive overhead heavy lifting and pushing.
As for the traumatic tears, the force and energy needed to create the tears becomes less and less as the patient gets older. Usually tears in younger patients (like 30’s to 40’s) are from high energy injuries like motorcycle, motor vehicle accidents or industrial accidents. As a patient gets older into their 60’s-70’s the trauma could be very minimal, like slipping and falling while grabbing onto something or falling down and landing on the shoulder.

How long does rotator cuff surgery take?
The surgery itself takes anywhere between 45 minutes to about an 1.5 hours depending on the size and extent of the tear, as well as the additional procedures that might also occur (like distal clavicle excision, biceps tenodesis, acromioplasty/decompression). The whole surgical day will take about 4 hours.
Usually patients arrive about 1 to 1.5 hours prior to surgical start time. The anesthesiologist and nurses will meet the patient. Surgery is done under general anesthesia, but is supplemented with a “Regional Block”. This is where the anesthesiologist will sedate the patient prior to going to the operating room, and using an Ultrasound Probe, they will localize the nerves coming out of the neck and into the shoulder, and place numbing medication in that area. This will allow for pain relief both during the surgery while the patient is asleep as well as pain relief after their surgery for about 12-18 hours. After surgery, the recovery time is between 45 minutes to 1.5 hours as well before the patient is fully awake, alert, taking oral fluids and/or food, and ready to go home.
Post-operatively, oral pain medication is prescribed. This is usually supplemented by some sort of ice administration (like ice pack, ice bags, or even Ice Machines that patients can buy or rent). The surgery is outpatient, and the patient goes home the same day.
Do you have to have surgery, or can a torn rotator cuff be healed with PT?
Once there is a full thickness tear, meaning a portion of the tendon is completely detached from the tuberosity (or bone), the tendon WILL NOT heal itself. This does not mean, however, that surgery is absolutely needed. Studies on atraumatic/nontraumatic tears show that about 70-75% people will improve and end-up avoiding surgery with proper measures, specifically and most importantly Physical Therapy. So while the tear itself does not re-attach to the bone, patient’s pain, function, strength and other symptoms will improve enough that surgery is not needed. The upside with this is that patients improve without surgery.
There is a small downside, and that is the larger the tear is at time of the start of the PT, the higher chance it is that the tear will progress in size and symptoms could worsen in the future, and thus require surgery down the road. This is not 100%, it is more like a range of 15-40% that the tear will get bigger and symptoms could worsen in the future, with the higher chance of progression the larger the tear size is.
What are the post-surgery protocols?
After going home, ice is recommended to the surgical area. Pain control is supplemented with anti-inflammatories and oral medication, usually some sort of narcotic. The narcotic is weaned off over the next 2-6 weeks after surgery.
The small incisions either have the sutures under the skin with bandaid-like strips called STERI-strips on the incisions, or the sutures are out of the skin with Nylon. Either way, there is also a bulky/thick dressing with tape over the incisions, and the bulky/thick dressings are removed at home 48-72 hours after surgery. After that happens, the patient can start getting the incisions wet. Generally, there is NO tub bathing or submerging the incisions under standing water, like pools, tubs, spas, beaches, until 3 weeks from surgery. If the patient had sutures outside the skin, these are removed at the first follow-up at 10-14 days post surgery.
The patient will be in a sling or a cradle that supports the arm and the repair immediately after surgery, and this is placed in the Operating Room while the patient is still asleep. Most standard post-operative protocols utilize the sling or cradle for 4-6 weeks. After going home, our office will call the patient the following morning to check on the patient, as well as answer any post-operative questions, and verify the follow-up appointment. Immediately, patients can come out of the sling to let the arm dangle while bending over, called a pendulum, and move the elbow, wrist, and hand so these joints do not become stiff.
Demonstration of shoulder pendulum swing
Formal Physical Therapy, or PT, does not start until after the first follow-up. The key, however, is not to have the patient ACTIVELY reach for 6 weeks, as the process of reaching out from the body or overhead will put too much tension on the repair, and if the shoulder is stressed too much in the early phase, this could lead to the repair not healing.
After the first follow-up appointment at 2 weeks from surgery, PT is started with PASSIVE motion. At the 6 week follow-up appointment from surgery, ACTIVE ASSISTED and progression to ACTIVE reaching and range of motion is started. Then, finally at 12 weeks, or around 3 months, STRENGTHENING is started.
How long would you have to go to physical therapy for after a rotator cuff surgery?
Therapy is ordered in sessions of 6 week blocks, usually 2-3 times per week for each 6 week block. On average, therapy lasts for about 3 months or 12 weeks. Sometimes, PT is extended past that time if patients have not turned the corner or regained full function by that time. PT is most important in the early stages when the shoulder is being moved by passive or active assisted range of motion. Once the strengthening phase starts, the frequency of visits can decrease and more of a home exercise program will be initiated.
How long will it take to resume my usual everyday activities with no pain?
Full unrestricted activity, with full strength and motion gains, along with no to minimal pain occurs on average between 5-6 months after surgery. Some patient will be earlier, some patients will take longer. There are studies that show, however, that while the majority of changes and improvements occur in the first 6 months, improvements in pain or soreness, motion, and strength will continue to improve up to 1 year after surgery.
How can I prevent future rotator cuff injuries?
The first key is to avoid known risk factors, like smoking, and lead a healthy lifestyle that limits chronic diseases, specifically disorders like diabetes. As for exercise and activities, if there is repetitive lifting or overuse type activities, especially if associated with pain, then stretching and strengthening with bands and pulleys a few times a week is essential to keep the rotator cuff tendons strong.
Also, it is good to not overtrain or work through pain if it is limiting quality of life or causing moderate to severe pain. Lastly, if there are concerns, even if there is no trauma, it is best to see one of our team members to be assessed.
Rotator cuff surgery FAQ
Do I have to wear a sling or a brace?
- Yes. Most protocols have patients wear a sling or brace for 4-6 weeks after surgery. Newer studies are suggesting that if the tear was small that a sling or brace is not needed after surgery, but not all surgeons have adopted this approach.
Will I need to stay at the hospital overnight after surgery?
- No. Over 90% of these surgeries will be done as an outpatient. Co-morbidities such as sleep apnea, pulmonary issues, advanced heart disease, or morbid obesity might require the patient to stay overnight in the hospital. This is usually decided based on the recommendation and instruction of the anesthesiologist involved.
How long does the surgery take?
- The surgery takes anywhere between 45 minutes to an 1.5 hours depending on the size and complexity of the tear.
How many follow-up appointments will I need to go to post-surgery?
- At a minimum there are 3 follow appointments: one at 2 weeks, then at 6 weeks, and then at 12 weeks from surgery. If the patient is still having issues, then additional office visits might occur after the 12 week mark.
When can I begin to drive again?
- Most recommendations are to avoid driving while in a sling and on narcotic pain medications after surgery. Most post-operative protocols utilize the sling for 6 weeks. The risk of driving while in the sling is that if a patient has to react to the road and they are in the sling, they might not be able to use the operative arm that is in the sling to control the steering wheel. Also, by virtue of wearing the sling, the surgeon is saying that the arm should not be used in activities such as driving, and if the patient takes the sling off to drive, this could lead to incomplete healing of the tendon. Lastly, we do not want the patient to be liable for an accident if they are driving in the sling and get in an accident. While these are the guidelines, many times patients do drive while in the sling; if it is absolutely necessary to drive, we recommend the patient to be as cautious as possible.
How much pain will I have while recovering from surgery?
- This is variable for everyone. The majority of patients take the prescribed oral pain medications, usually narcotics, for the first few days up to the first follow-up appointment. Occasionally, this or a less strong pain reliever will be renewed at the first follow-up. On the night after surgery, as the regional block wears off and the patient is at home, there sometimes is a rebound of the pain. We recommend patients stay ahead of that, and not only use ice and other medications, but take the pain medication before that happens, usually when the patient starts to have their arm “wake-up” from the block, but before they sense pain. Once the patient makes it through the first night, the pain slowly improves every day, with the goal of minimal pain medication use by the first follow-up.

Dr. R. Bryan Butler is an orthopaedic surgeon with an interest in specialized care for injuries of the Shoulder and Elbow. After earning his medical degree from the University of Maryland School of Medicine, he spent his residency at the University of Maryland Medical Center and R Adams Cowley Shock Trauma Center where he was involved in research, education, lectures, and served as Academic Chief Resident in his final year of residency. Dr. Butler continued his training at the Harvard Combined Orthopaedic Fellowship Program, internationally with the world renowned shoulder surgeon Dr. Laurent LaFosse, and received further sub-specialty training in Elbow Surgery at the Mayo Clinic in Rochester, Minnesota. Full Bio