What is Platelet-Rich Plasma (PRP) Therapy?
Platelet-Rich Plasma, or PRP, is produced from your own blood. This procedure involves collecting a sample of your blood and spinning it in a centrifuge to separate the platelets. Blood is made up of 4 main components: plasma, red blood cells, white blood cells, and platelets. The platelets are the cells in our body that contain growth factors, which stimulate the normal wound healing process, e.g. the same way that your skin heals after a scrape. With PRP, you create a supra-therapeutic level of your own platelets (over 500% more platelets than normal blood) so that you heighten the healing of a chronically injured tissue. The concentrated platelet rich plasma is then injected back into the injured area to stimulate healing and regeneration. All PRP injections are done under ultrasound guidance to confirm placement of the PRP in the correct tissue.
The platelets contain healing agents, or “growth factors.” Let’s look at some of the growth factors and what they do:
- Platelet-derived growth factor (PDGF) is a protein that helps control cell growth and division, especially blood vessels. When more blood (and the oxygen it carries) is delivered to the site of a wound, there is more healing.
- Transforming growth factor beta (or TGF-β) is a polypeptide and is important in tissue regeneration.
- Insulin-like growth factors are signaling agents. They help change the environment of the damaged joint from diseased to healing by “signaling” the immune system to start rebuilding tissue.
- Vascular endothelial growth factor (VEGF) is an important protein that brings healing oxygen to damaged tissue where blood circulation might be damaged or inadequate.
- Epidermal growth factor plays a key role in tissue repair mechanisms.
Frequently Asked Questions about Platelet-Rich Plasma Therapy:
Is PRP indicated for me?
PRP therapy is indicated for injuries that have failed to heal despite traditional treatment options as well as for chronic degenerative conditions. It is a viable non-surgical option to help aid in healing tissue. It can be performed in any musculoskeletal structure, including muscles, tendons, and joints all over the body. Some examples include: partial tendon tears, muscle strains, articular cartilage injury, mild to moderate osteoarthritis, and chronic tendon injuries.
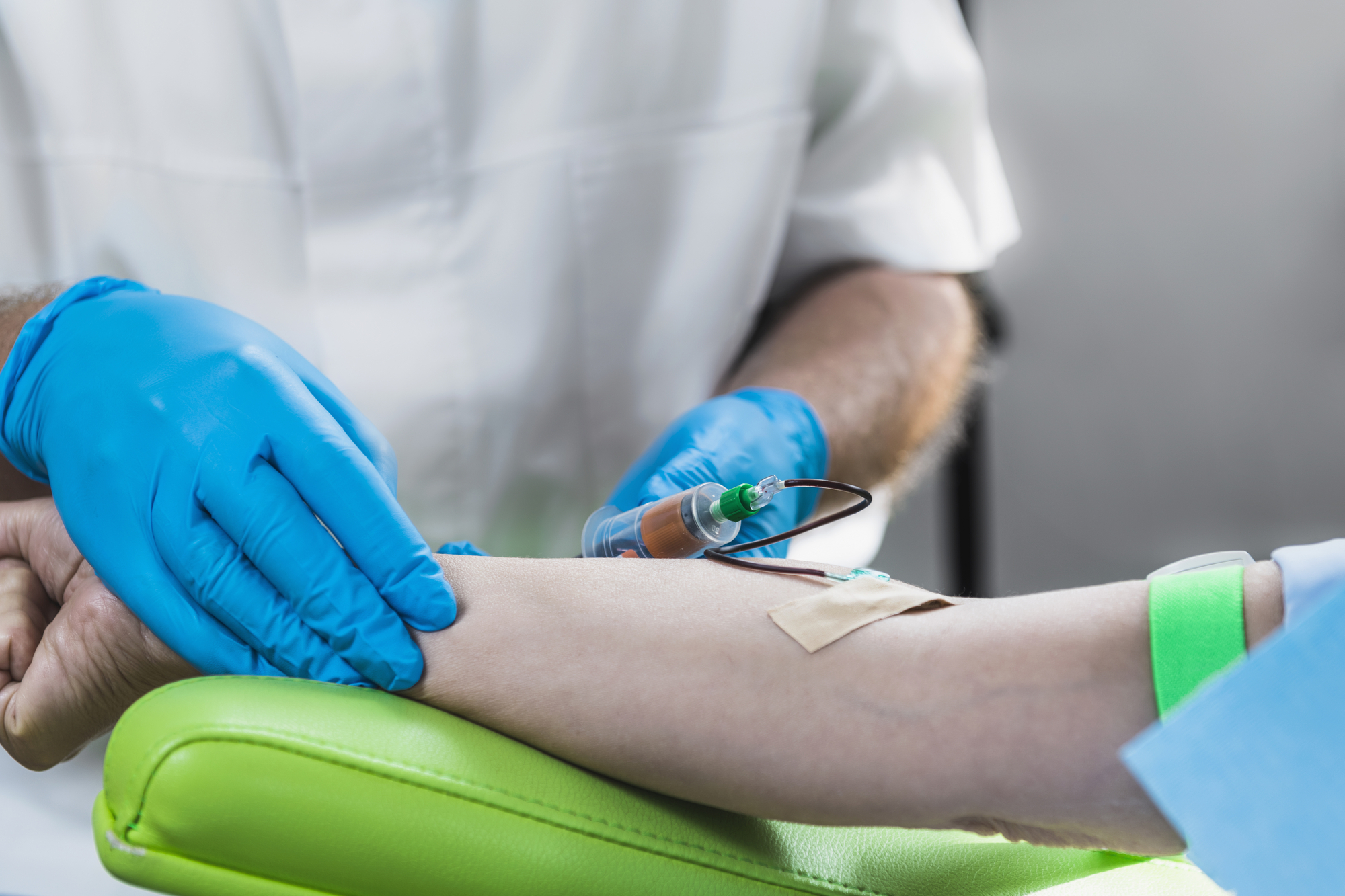
How is PRP made?
To prepare PRP, blood is taken from your arm with a special kit similar to a normal blood test. It is then placed in a special centrifugation machine that separates the platelets from the blood in order to be extracted in a concentrated form called PRP. The entire PRP Therapy takes about 30-45 minutes.
How many treatments are necessary?
This can vary depending on the condition which we are treating. For some conditions patients can achieve successful outcomes with only one injection. In some cases, a series of three injections is required to achieve significant results. Each injection is spaced 1-2 weeks apart. There is no limit to the number of treatments you can have; however, literature has shown that about 15% of patients do not see improvement with more than three injections and should consider other treatments.
Are there any side effects with platelet-rich plasma therapy?
Since your own blood is used, there is no risk for transmitted blood-infections. PRP has a strong antibacterial effect so risk of local infection is minimal. It is normal to have increased soreness or pain after the procedure for an average of three days. We will offer you a medication plan to help with this.
Will my insurance pay for this treatment?
Since this is a fairly new procedure, most insurance companies have not incorporated it yet to their list of approved procedures and do not consider this to be a reimbursable expense. While there is growing literature to support the use of PRP as a viable therapy with patient improvements and benefits, the insurance companies still classify this treatment as “investigational” of “experimental” and thus will not cover.
What are the potential benefits of Platelet-Rich Plasma?
PRP stimulates healing of the injured tissue by activating your body’s natural healing capacity. Patients on average report more than 50% improvement in 6 weeks and up to 100% improvement in 12 weeks. This may eliminate the need for surgical interventions in some cases. In addition, PRP Therapy is a minimally-invasive procedure that is done in the clinic; therefore, you go home the same day.
What can I do after my Platelet-Rich Plasma injection? Can I resume exercises, sports, work?
While PRP injections are minimally invasive, non-surgical procedures, it is important to remember that this is still a procedure! In order to achieve the proper tissue healing response that the injections can provide they must be accompanied by the proper after care including initial rest, avoidance of NSAIDs and exercise, and the initiation of a dedicated physical therapy program about 1-2 weeks after the last injection. The healing response initiated by the injections needs to be accompanied by the correct rehabilitation plan to maximize full healing and achieve improved function. Ignoring the therapy after the injection will likely lead to suboptimal results. Remember this is not a quick-fix and will take up to 3 months to complete the rehabilitation process and see the full potential benefits.
Pre-Procedure Instructions
- Stop anti-inflammatory (NSAIDs) medications 5 days prior to procedure (e.g. ibuprofen, naproxen, celebrex, etc.).
- You cannot be on any blood thinners (Coumadin, Eliquis, Xarelto, Plavix, Pradaxa) before your injection. You must clear stopping any of these medications with your cardiologist before being considered a candidate for PRP injection.
- Make sure to drink plenty of water pre-procedure, up to 1 gallon, if possible. This assists with the ability to draw adequate blood for your procedure.
- Depending on the condition we are treating, you may be asked to perform 15-20 minutes of exercise prior to your procedure as some literature suggests increased growth factors in samples after exercise. Plan to spend at least 45 minutes to over an hour at the clinic for your procedure.
- If you are concerned about driving home after your procedure, bring a family member or friend for your appointment.
Post-procedure Instructions
- We recommend having someone drive you home after the procedure.
- Blood thinners (e.g. Aspirin, Plavix, Coumadin, etc.) may be resumed 24 hours after the procedure.
- Avoid anti-inflammatory medications for six weeks after the procedure (e.g. ibuprofen, naproxen, celebrex, etc.).
- Increased irritation in the affected area may occur after your PRP injection. This is part of the healing process. Ice the affected area three to four times per day for 15 minutes for the next three days. You may take Extra Strength Tylenol as needed for pain.
- You may experience an increase in pain and soreness after the numbing wears off for 2-5 days after your treatment. The initial inflammatory phase lasts 7 days and the secondary phase can last up to 14 days.
- If you develop fever, persistent redness and swelling at the site of injection, call the office at 813-684-2663. These may be a sign of infection.
- The most important part of the PRP Therapy is that you follow the Post-procedure instructions in order to optimize the healing of the tissue and decrease the risk of causing further damage. Limit movement of the treated area for the first three days after the procedure. Avoid lifting or any strenuous activity for the first seven days. If a splint was provided, you should wear it during the first 7 days. A post-PRP rehabilitation program will be provided to you to complete with your physical therapist. On average, sports-related drills are begun at 8 weeks from the procedure, and return to play of sports without restrictions usually occurs at 12 weeks from the procedure.
Post-PRP Rehabilitation Protocol
|
Phase |
Length of Time |
Restrictions |
Rehabilitation |
| Phase I
Tissue Protection |
Day 0-7 |
|
|
| Phase 2
Early tissue healing, collagen formation |
Days 8-14 |
|
|
| Weeks 2-6 |
|
|
|
| Phase 3
Collagen strengthening |
Weeks 6-12(+) |
|
|

Dr. Mark Sando is an internationally recognized orthopaedic surgeon specializing in sports medicine, arthroscopy and injuries of the shoulder, knee and hip. He earned his medical degree from Case Western Reserve University School of Medicine and completed residency at the University of Maryland Medical Center and R Adams Cowley Shock Trauma Center. After residency, Dr. Sando went on to complete subspecialized training in Sports Medicine as a fellow at the prestigious Kerlan-Jobe Orthopaedic Clinic in Los Angeles, CA under the direction of Dr. Neal ElAttrache. He has worked with numerous college athletic programs and professional teams including the world champion Los Angeles Kings, Los Angeles Lakers, Los Angeles Dodgers, and Los Angeles Sparks. Dr. Sando has been with the Orthopaedic Medical Group of Tampa Bay since 2015. Full Bio